TEPEZZA can help patients regardless of disease activity or duration1-4
79-year-old male patient, living with TED for 2 years
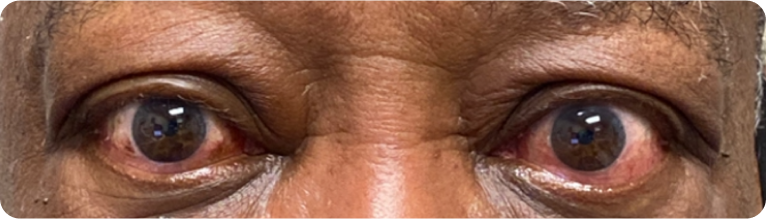

Visible signs:
Proptosis (28 mm OD; 25 mm OS), eyelid swelling, conjunctival redness
Nonvisible symptoms:
Intermittent diplopia
Impact on daily living:
Difficulty reading, lowered self-esteem
See the Burden-Impact Model for this patient
See an example
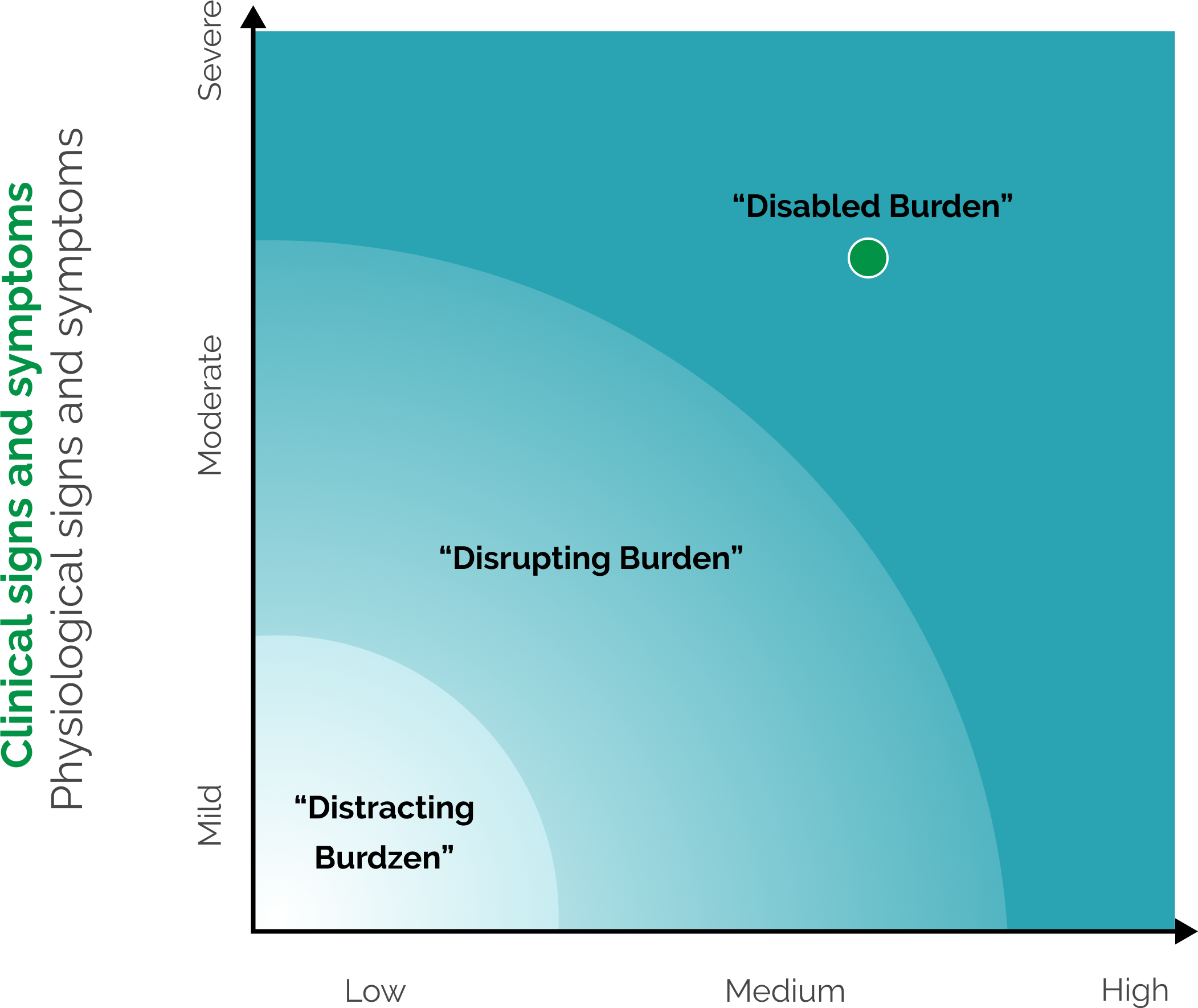

Patient-Reported Impact
Degree to which symptoms impact patients’ daily activities and emotional well-being
Not an official medical tool.
79-year-old male patient, living with TED for 2 years


Visible signs:
Proptosis (24 mm OD; 22 mm OS)
Nonvisible symptoms:
Diplopia resolved
Daily living:
“I’ve been treating patients with TEPEZZA since 2020 and it has had a huge impact.” – Amina Malik, MD
See the Burden-Impact Model for this patient
See an example
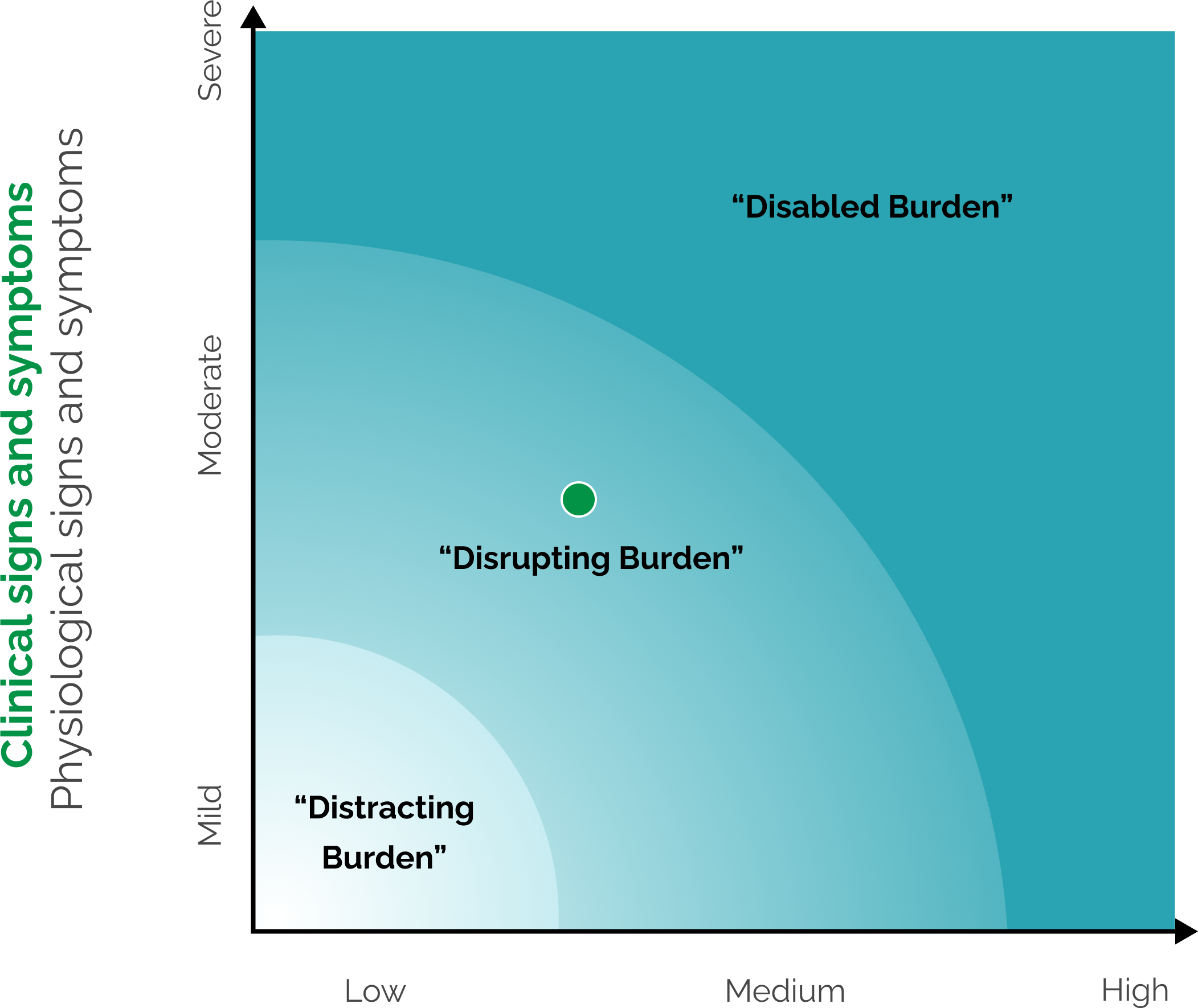

Patient-Reported Impact
Degree to which symptoms impact patients’ daily activities and emotional well-being
Not an official medical tool.
55-year-old male patient, living with TED for 20 years


Visible signs:
Proptosis (22 mm OD; 23 mm OS), eyelid swelling, conjunctival redness
Nonvisible symptoms:
Constant diplopia, eye pain, and burning sensation
Impact on daily living:
Lowered work productivity due to diplopia; reduced self-esteem
See the Burden-Impact Model for this patient
Orbital MRI of a long term patient with TED from the Phase 4 Study3
Patient had TED for 7 years
Baseline
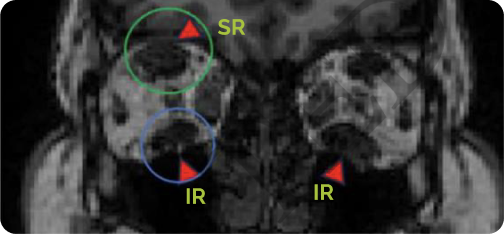

Post treatment (at Week 24)
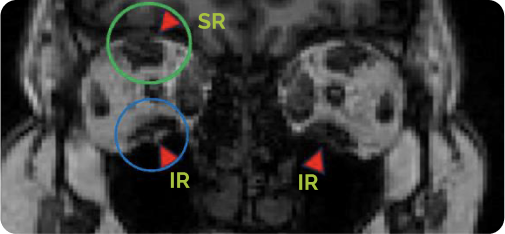

The blue and green circles point to a coronal view of the inferior and superior rectus muscles (IR and SR), respectively.
See an example


Patient-Reported Impact
Degree to which symptoms impact patients’ daily activities and emotional well-being
Not an official medical tool.
55-year-old male patient, living with TED for 20 years


Visible signs:
Proptosis (20 mm OD; 21 mm OS)
Nonvisible symptoms:
Intermittent diplopia, eye pain and burning sensation resolved
Daily living:
Patient reported improvement in daily activities; happy with results
See the Burden-Impact Model for this patient
Orbital MRI of a long term patient with TED from the Phase 4 Study3
Patient had TED for 7 years
Baseline


Post treatment (at Week 24)


The blue and green circles point to a coronal view of the inferior and superior rectus muscles (IR and SR), respectively.
See an example


Patient-Reported Impact
Degree to which symptoms impact patients’ daily activities and emotional well-being
Not an official medical tool.
TEPEZZA has been shown to be effective in patients with TED with a wide range of clinical manifestations3,4
Because each patient responds differently to treatment, it is important that patients complete the full TEPEZZA treatment course of 8 IV infusions as studied in clinical trials1
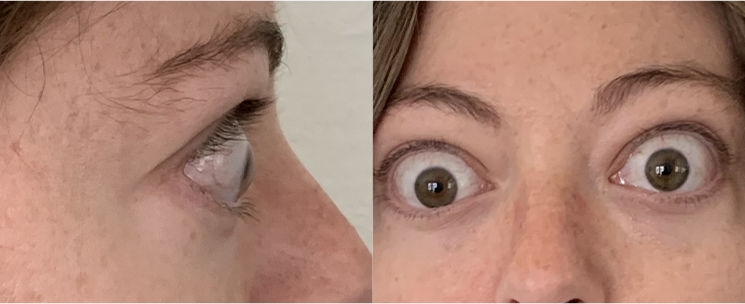

BASELINE
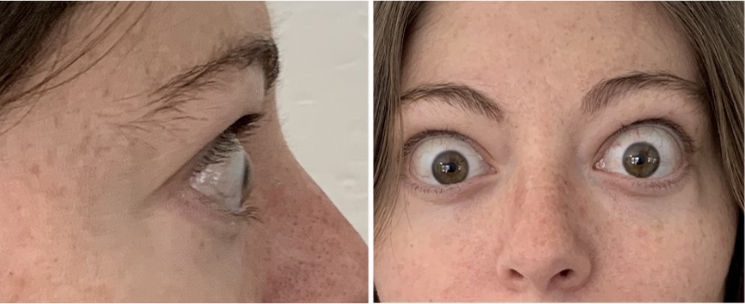

INFUSION 2
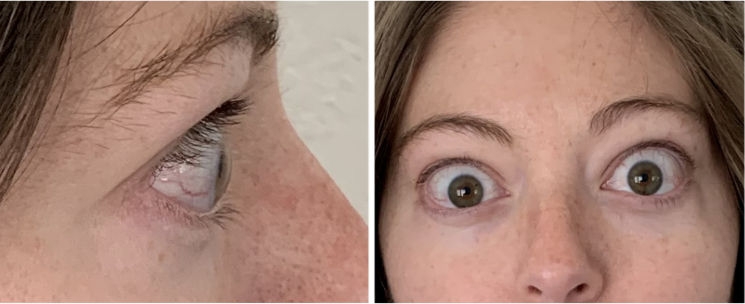

INFUSION 3
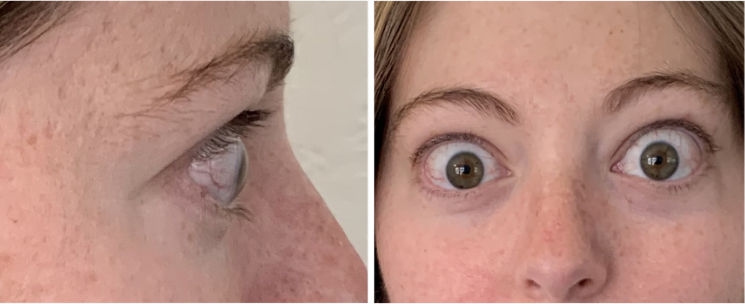

INFUSION 4
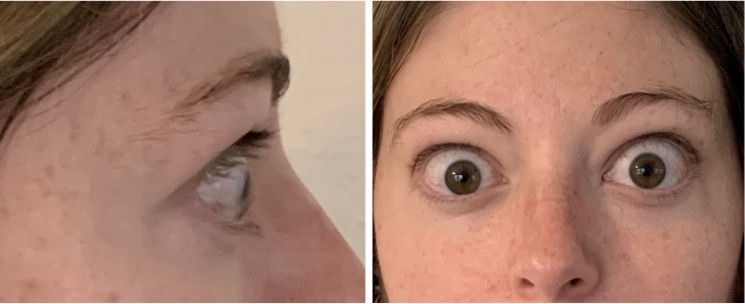

INFUSION 5
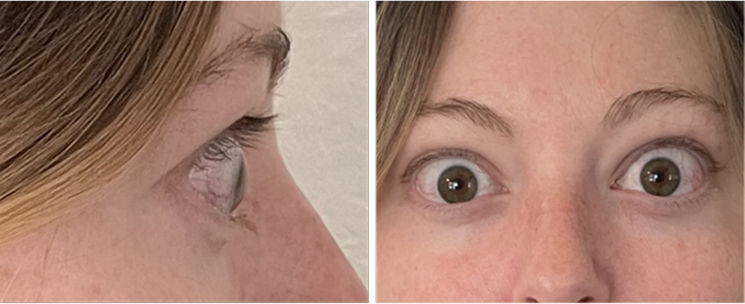

INFUSION 6
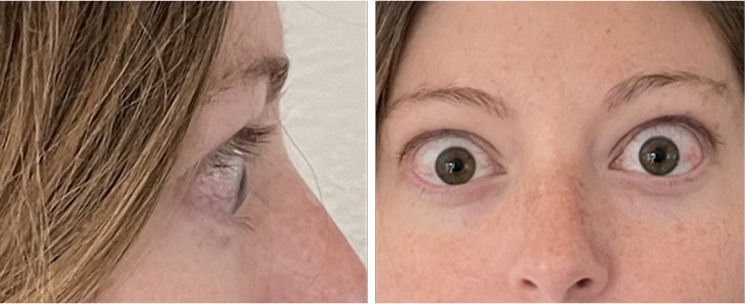

INFUSION 7
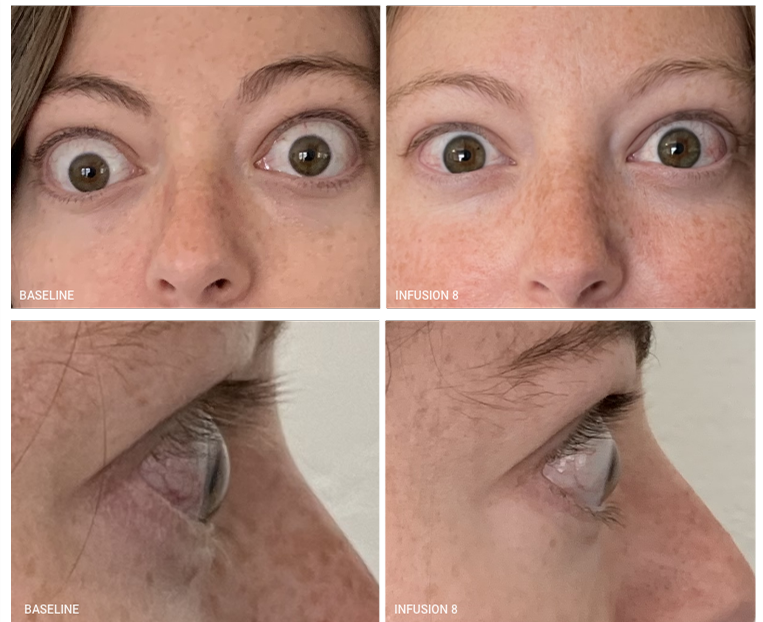

BASELINE COMPARED WITH INFUSION 8
A full course of treatment with TEPEZZA is 8 IV infusions—one every 3 weeks. In the Phase 3 study, improvement of proptosis as measured by mean change from baseline was observed as early as 6 weeks and continued to improve through Week 24.1
Cases of patients with TED and their individual experiences with TEPEZZA. Individual results may vary. Clinical presentations represent a range of patients with TED. Patients with prior surgery or orbital radiation treatment for TED, history of compressive optic neuropathy, and concomitant steroid use were excluded from clinical trials for TEPEZZA.2-4
IGF-1R, insulin-like growth factor-1 receptor; IV, intravenous; MRI, magnetic resonance imaging; OD, oculus dexter; OS, oculus sinister; TED, Thyroid Eye Disease.
Receive the latest news and updates about TEPEZZA
Receive the latest news and updates about TEPEZZA











